Osteopathy to treat mental health issues
Osteopathy to treat mental health issues
Millions worldwide suffer from chronic musculoskeletal back pain (lasting over three months). The issue is so large that in the UK alone, it’s estimated that 116m days of work are missing, a million hospital appointments are created and five million GP visits are scheduled – only for low back pain.
The physical agony is frequently not a standalone issue, however. 35 percent of individuals who suffer from low back pain can also be diagnosed with depression, anxiety and social isolation.
NICE guidelines imply that chronic back pain sufferers should have physical treatment as part of a wider package of treatment which includes psychological assistance. But we have been researching how one type of osteopathic treatment may be used to treat both bodily and psychological ailments.
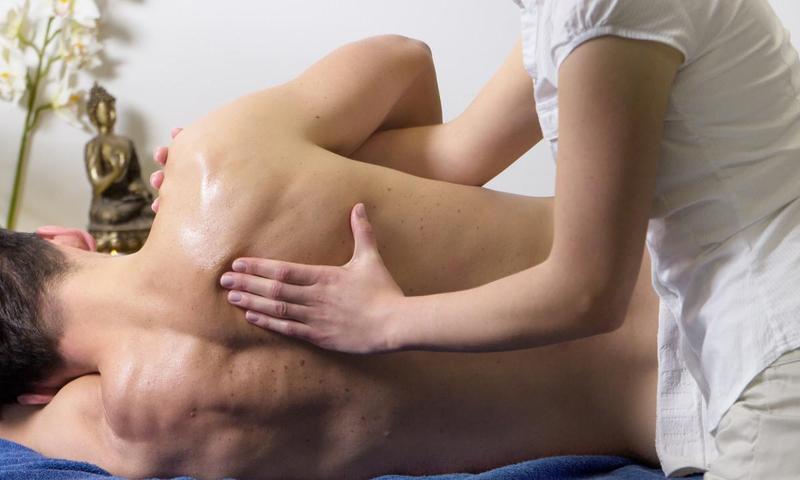
Osteopathic manipulative treatment is a drug-free medical system which utilizes touch-based massage, manipulation of soft tissue and joints, and spine mobilisation procedures, to diagnose and treat pain related conditions. Practitioners utilize a structured evaluation to discover malfunction relating to the skull, spine, pelvis and abdomen, in addition to upper and lower limbs, and target treatment.
OMT has been discovered to work for many kinds of muscoskeletal pain, for example chronic neck pain. Moreover, it’s been demonstrated to be more powerful than the standard primary care choices – such as painkillers and exercise – in improving quality of life for anyone who have persistent low back pain and 12 months into therapy.
Scientists also have demonstrated that OMT can decrease subacute (between chronic and acute ) lower back pain. Accordingly, spinal mobilisation and manipulation alone have been found to be effective for acute, subacute and chronic low back pain.
Even though this is all very positive, there’s a pattern . The limited OMT studies have focused largely on physical issues, not the related mental health problems.
Fixing mental health problems
To discover more about the way osteopathy could affect mental health, at our university health and well-being academy, we’ve recently conducted among the earliest studies about the emotional effect of OMT -- with favorable outcomes.
Spine mobilisation.
Photographee.eu/Shutterstock
For the previous five years, therapists in the academy have been using OMT to deal with members of the public who suffer from many different musculoskeletal disorders which have resulted in chronic pain. To discover more about the emotional health effects of this treatment, we looked at three different points in time – before OMT treatment, following the first week of therapy, and after the second week of therapy and asked patients how they felt using mental health questionnaires.
This information has proven that OMT is effective for reducing anxiety and psychological distress, in addition to enhancing patient self-care. However, it may not be suitable for all mental disorders associated with chronic pain. For example, we discovered that OMT was less effective for depression and fear avoidance.
All is not lost, though. Our results also implied that the positive emotional effects of OMT may be further enhanced by mixing it with treatment approaches like acceptance and commitment therapy (ACT). Some research indicates that emotional issues like stress and depression are related to inflexibility, and contribute to experiential avoidance. ACT has a positive impact at reducing avoidance, therefore may be helpful with reducing the fear avoidance and depression (which OMT didn’t substantially decrease ).
Other researchers have also implied this joint approach might be practical for some subgroups getting OMT where they may accept this therapy. And, further backing this idea up, there has been one pilot clinical trial 30083-9/abstract) and a feasibility analysis that have utilized ACT and OMT with some success.
Be the first to post a message!