Every Time You Fly on a Plane You Are Exposed to Toxic Chemicals. Here is How to Recover
Every Time You Fly on a Plane You Are Exposed to Toxic Chemicals. Here is How to Recover
Over the last 9 years, I have traveled around the country and the world teaching people how to use diet and lifestyle to restore health. However, all that travel created a problem for me. Often, for the next 24 to 48 hours after I’d flown somewhere, I’d experience a flare of my neuropathic pain and increased spasticity.
It got worse and worse, and I started to think I’d have to stop doing events that required flying. Fortunately, my functional medicine physician and I were able to figure out why flying was causing me so much trouble.
Depending on the model of the aircraft, vaporized jet fuel is recirculated in the internal cabin. That means the flight crew and passengers are exposed to jet fuel. That jet fuel must be metabolized by your liver and kidneys and then excreted in bile and urine.
Depending on the efficiency of the enzymes in your detoxification pathways, you might easily excrete all the jet fuel to which you are exposed. But if a person’s detoxification enzymes are less efficient, the jet fuel accumulates in their fat cells.
The accumulated jet fuel (along with other pollutants) increases the level of inflammation in the brain and the body, which increases pain, fatigue, and malaise. The good news is that boosting enzymes is possible and has eliminated the problems I had that were likely associated with my body’s inefficient handling of jet fuel. Now that I know how to take care of myself, flying is much more comfortable.
5 Strategies To Reduce Symptoms of Exposure To Jet Fuel
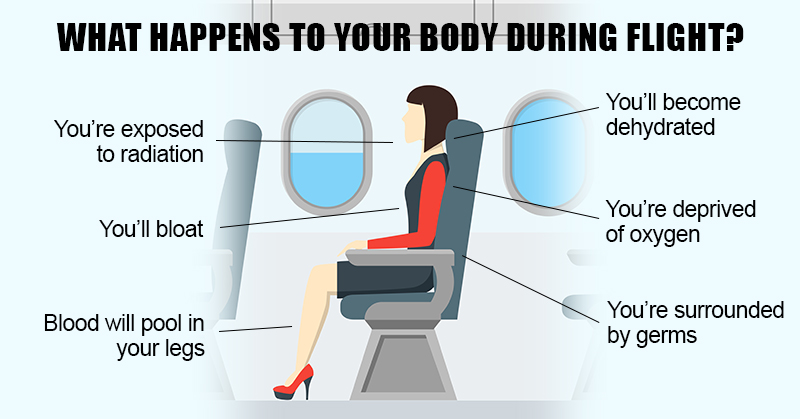
Many of you probably find that flying leaves you more vulnerable to headaches, body aches, viral infection, or a flare of your underlying health issues. Here are some strategies to reduce the accumulation of jet fuel and accompanying symptoms:
1. Increase the production of bile
You can increase bile by consuming calendula tea or detox tea that includes burdock root, dandelion root, or dandelion leaf. Beetroot will also increase bile production. I carry a variety of detox teas with me when I travel. I also carry beet powder, which helps me get enough color into my diet, and powdered coconut milk, which I add to my tea. It contains fat, which also increases bile release.
2. Increase the protection of the liver cells doing the detoxification work
Detoxification can be stressful to the liver cells. Their work will be easier if they have a better supply of intracellular antioxidants (glutathione). Milk thistle extract provides significant support to liver cells by increasing intracellular glutathione, so take 100 mg to 300 mg one to three times a day while you travel.
Also helpful is a dose of N acetylcysteine (NAC) — between 500 mg to 2 grams per day — as well as 500 mg to 2 grams a day of vitamin C.
3. Use a toxin binding agent
Water-soluble toxins in the bile get dumped into the small intestine. The small intestine reabsorbs bile because bile is so valuable to the body. That means the toxins are recycled and are hard to fully eliminate. But you can add a toxin binding agent – which will bind to the toxins in the bile and keep them from being reabsorbed.
Algae from chlorella or will bind to toxins so they are excreted in your next bowel movement. To this end, I add 2 to 5 grams of algae to my daily regimen. Another option would be activated charcoal, which is very effective at binding toxins. But activated charcoal is constipating. You will need to take more fiber or magnesium to keep from getting constipated.
4. Feed your microbiome
The bacteria in the bowels are responsible for metabolizing and excreting approximately 25% of the toxins you are exposed to each day. So pay attention to your bowels! Eat 6 to 9 cups of vegetables every day to provide enough fiber to hit the goal of passing two soft stools each day.
If the vegetables are not enough, add more fiber — seed puddings are a tasty way to increase fiber intake. Keep increasing the fiber until you are having soft, snake-like bowel movements twice a day.
5. Follow the Wahls Diet
The diet includes 6 to 9 cups of green leafy vegetables, deeply pigmented vegetables, and sulfur-rich (cabbage family, onion family, or mushroom family) vegetables each day. This balance of vegetables will maximize your cellular function and your ability to stay healthy.
In summary, providing more support to your liver as it eliminates toxins will markedly improve your ability to process and eliminate jet fuel and other pollutants in your life.
It will improve the tolerance you have for air travel, and will likely also help you slowly decrease the level of solvents as well as the various plastics, heavy metals, and fragrances stored in your fat that can disrupt hormones and interfere with thyroid and sex hormone balance. In other words, tuning up your detoxification pathways will make travel easier and probably improve your health overall.
My book, , details the food plan and protocol that I used for my recovery, in my clinical trials, and in my clinic. The protocol will markedly boost the efficiency of the enzymes that process and eliminate the chemicals stored in your body.
Here is a recipe I use to boost the efficiency of my liver to process and eliminate jet fuel while I am traveling. You will find more recipes to boost your detoxification pathways in my new cookbook, .
Bile Boosting Ginger Calendula Tea
Ingredients:
¼ inch grated fresh ginger
2 teaspoon
1 teaspoon (or to taste)
2 cups boiling water
Instructions:
Brew the calendula tea and fresh ginger with boiling water for 10 minutes.
Strain and add coconut milk to taste.
The ginger and calendula will increase the production of bile, which boosts detoxification in the liver. The addition of 500 mg or more of chlorella taken at the same time will further support detoxification, increasing the liver’s production of bile and the body’s ability to eliminate the various pollutants that are stored in your fat, such as plastics, solvents, and pesticides and heavy metals like lead, mercury, and arsenic.
The beauty of this tea is its very pleasant taste and its effectiveness at improving the efficiency of your liver.
This post is written by Dr. Terry Wahls, a clinical professor of medicine at the University of Iowa. She is the author of
Be the first to post a message!
