Trans-cranial Magnetic Stimulation to Alleviate Addictions
Trans-cranial Magnetic Stimulation to Alleviate Addictions
According to government figures, 21.5 million Americans suffer from a substance abuse disorder, alcoholism being the most frequent. As of 2014, 64,000 lost their lives to some type of overdose. Although a lot of treatment alternatives are available, whatever the sort of dependence, recidivism rates are extremely high. Currently, researchers at the Medical University of South Carolina think they could reboot the brain’s reward center and halt addiction. This is achieved through something called repeated trans-cranial magnetic stimulation (rTMS). What’s TMS and has it been demonstrated to assist those gripped by addiction?
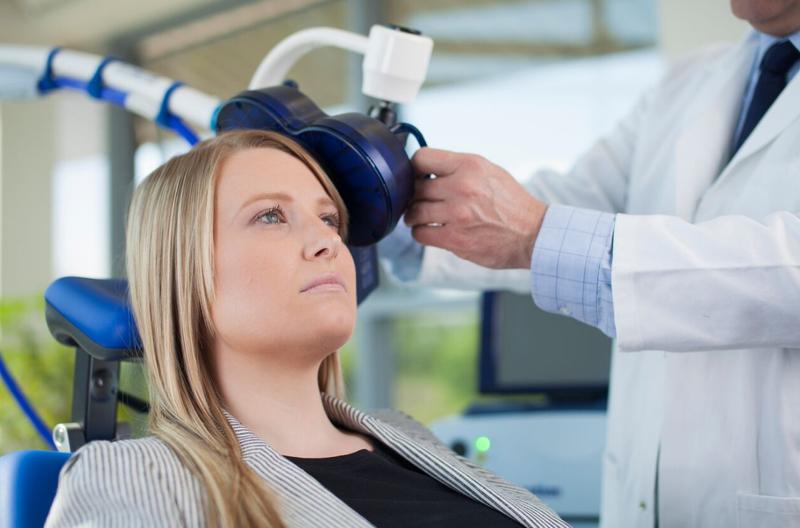
TMS is a noninvasive procedure in which a coil is placed on the scalp, which passes magnetic impulses through the skull. It’s believed that a varying magnetic field applied to specific areas of the brain increases coherence between cortical regions–basically improving communication between distinct brain areas. The FDA accepted this procedure a decade ago to help alleviate the symptoms of depression when antidepressants didn’t get the job done.
The frequency exerted during TMS may be as high as 10-20 Hertz or as low as 1 Hertz, depending on an individual’s motor threshold. Motor threshold is set by how much frequency must make a patient’s leg or thumb jump, when TMS is placed on the brain’s motor strip. It does not hurt. Patients report feeling a tapping sensation on the head. Sessions last 30 minutes and generally, therapy occurs a few times a week for six weeks.
As it is applied to the scalp, deeper regions of the brain cannot be reached. But, TMS has shown to assist people that have depression by stimulating part of the brain called the prefrontal cortex. Physicians are considering TMS for different ailments too, such as Parkinson’s, epilepsy, chronic pain, and schizophrenia. While brain stimulation has been used for decades to deal with psychiatric disorders, only recently have scientists been experimenting with TMS to deal with addiction.
The idea was inspired by a 2013 National Institute on Drug Abuse (NIDA) study, headed by neuroscientists Antonello Bonci and Billy Chen. They used rats who were addicted to cocaine, they would risk a series of painful electric shocks in order to receive their fix. The rodents had been altered, which makes the neurons in their brains responsive to light. When the scientists stimulated the region of the brain known for impulse control, the rats could kick the habit instantly. Bonci in the paper wondered if TMS may have a similar impact.
Luca Rossi–an Italian doctor addicted to crack cocaine along with his father, a chemist, after learning of the study, chose to approach Italian addiction specialist Luigi Gallimberti with the idea. Since then, Gallimberti’s laboratory has treated more than 300 addicts with TMS. For addiction, normally the ventromedial prefrontal cortex, the reward centre of the brain, is stimulated. This is considered to be where addiction originates from. Regrettably, we don’t know all of the intricacies of how addiction impacts the mind. Because of this, there is no present treatment based on altering the neural circuit accountable for addiction, yet.

The ventromedial prefrontal cortex is the place of the brain’s reward centre and therefore, is accountable for addiction. Image credit: National Institutes of Mental Health (NIMH).
One thing we do understand is that addiction hijacks the brain’s reward circuit. It floods the brain with dopamine–that gives us warm, euphoric feeling. Because of this, the brain’s dopamine receptors become accustomed to being flush with the feel good neurotransmitter. After awhile they get used to getting a specific amount, a tolerance is built up, and thus the individual wants more and more simply to get exactly the exact same result, leading to dependence. Currently, researchers in Medical University of South Carolina are the first to illustrate that TMS can decrease brain activity related to addiction in cases of chronic alcohol and cocaine misuse. These findings were published in the journal Biological Psychiatry: Cognitive Neuroscience and Neuroimaging. 30080-6/abstract “Biological Psychiatry “)
Researchers carried on two concurrent studies. Study author Tonisha Kearney-Ramos, Ph.D. led these, which were supervised by senior author Colleen Hanlon, PhD. The first part comprised 24 alcoholics and the next, 25 cocaine addicts. Each underwent an actual TMS session and a one, where investigators pretended to administer TMS, but didn’t really turn on the device. Scientists took brain scans with an fMRI before and after TMS occurred, to rate each participant’s reaction to medication or alcohol cues, such as being shown a liquor bottle.
Many times, brain activity in the ventromedial prefrontal cortex gets raised once the individual witnesses something associated with their addiction. This is known as cue reactivity. When they underwent bona fide TMS, participants revealed less cue reactivity than following the sham session. What remains to be seen yet, is whether these changes lead to decreased alcohol or drug usage. According to the investigators, repeated TMS sessions may do the job. Cue reactivity is a huge part of a lot of different ailments too, such as anxiety, PTSD, and traumatic brain injury. TMS might have the ability to assist these patients too.
To Find out More about TMS, click here:
Be the first to post a message!